These medications can be used as the patient is being prepared for pacing (in an effort to prevent the patient from declining) and should be titrated based on the patient’s response. 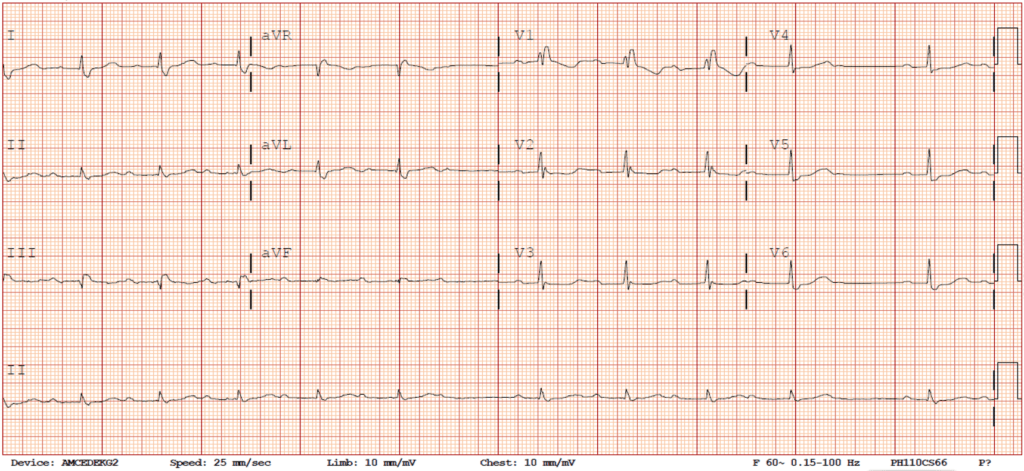
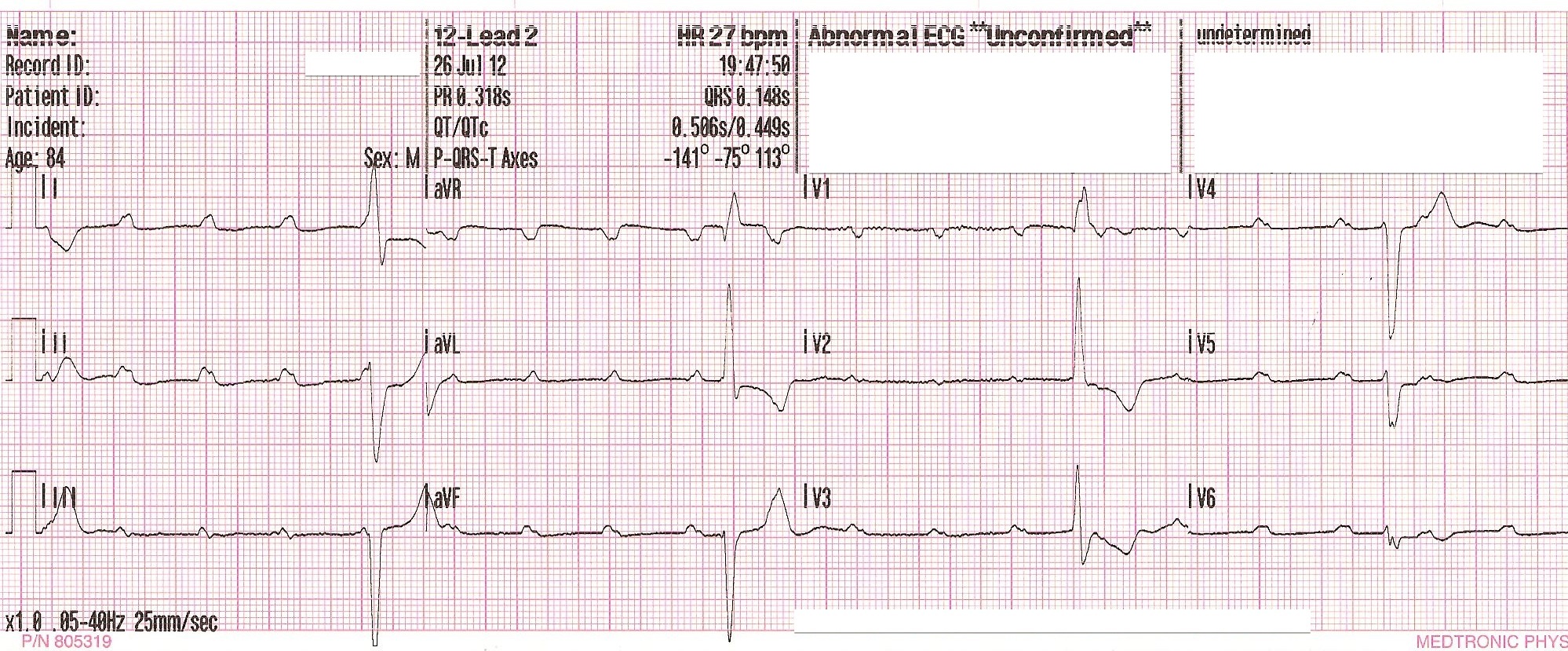
The ACLS Adult Bradycardia Algorithm indicates that dopamine can be administered via IV infusion at 5-20 mcg/kg per minute, or, epinephrine may be administered via IV infusion at 2-10 mcg/minute. However, when the patient does not respond to the administration of atropine, these medications can be used as alternatives. Beta-adrenergicsĭopamine and epinephrine infusions are not considered first-line treatments for unstable bradycardia. If the atropine is not effective, the healthcare provider can administer beta-adrenergic medications while concurrently preparing the patient for pacing. Although atropine is indicated as a first-line medication in the ACLS Adult Bradycardia Algorithm, patients with a second-degree AV block type II may not respond to this medication or it may worsen the heart block, increasing the risk for clinical deterioration to a complete heart block or ventricular asystole. Medications Atropineįor the patient with poor perfusion due to a consistent second-degree AV block type II, the ACLS Adult Bradycardia Algorithm recommends starting with 1mg of atropine administered intravenously, which can be repeated every 3-5 minutes, up to a total dose of 3mg. Depending on the patient’s clinical condition and response (or lack thereof) to treatment, it may be necessary to move quickly through the treatment options outlined within the ACLS Adult Bradycardia Algorithm to prevent the patient from experiencing cardiac arrest. In determining that an adult patient is symptomatic with a consistent bradyarrhythmia (such as a second-degree AV block type II) and displays signs and symptoms of poor perfusion (as previously described), the healthcare provider should utilize the ACLS Adult Bradycardia Algorithm to guide treatment. The healthcare provider should also assess and identify potential causes for the patient’s clinical condition by evaluating H's and T's during this initial phase of care. Intravenous access should be obtained, as well as a 12-lead ECG, if possible. Initial steps the healthcare provider should take in caring for a patient, according to the Advanced Cardiac Life Support (ACLS) Primary Assessment, are to manage the patient's airway, provide supplemental oxygen if needed, determine the patient's cardiac rhythm, and monitor vital signs. Treatment of Second-Degree AV Block Type II Autoimmune conditions (such as systemic lupus erythematosus).Inflammatory conditions (such as Lyme disease).Medications, such as digoxin, calcium channel blockers, or beta blockers.Infiltrative cardiomyopathies (such as hemochromatosis, amyloidosis, sarcoidosis).Patients exhibiting this heart dysrhythmia often have underlying heart disease. This type of heart block may be attributed to structural damage within the AV conduction system of the heart. What Causes a Second-Degree AV Block Type II? A regular pattern of blocked atrial depolarizations (P waves) may occur before conduction to the ventricles (QRS complex) is achieved, demonstrated by a recurring P: QRS ratio of 2:1 or 3:1 (or more)Ī patient with a second-degree AV block type II may exhibit:.When present, QRS complex is often wide.Atrial rate is regular, ventricular rate is bradycardic (What are the ECG Characteristics of a Second-Degree AV Block Type II? A second-degree AV block type II is an unstable warning rhythm that can lead to a complete heart block (third-degree AV block) or ventricular asystole without proper identification and treatment. This bradycardic rhythm is identified through an electrocardiogram (ECG) and is caused by an irregular block of atrioventricular conduction below the AV node. Identifying and Treating Second-Degree AV Heart Block Type II What is a Second-Degree AV Block Type II?Ī second-degree atrioventricular (AV) block type II is also known as Mobitz type II second-degree AV block. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
